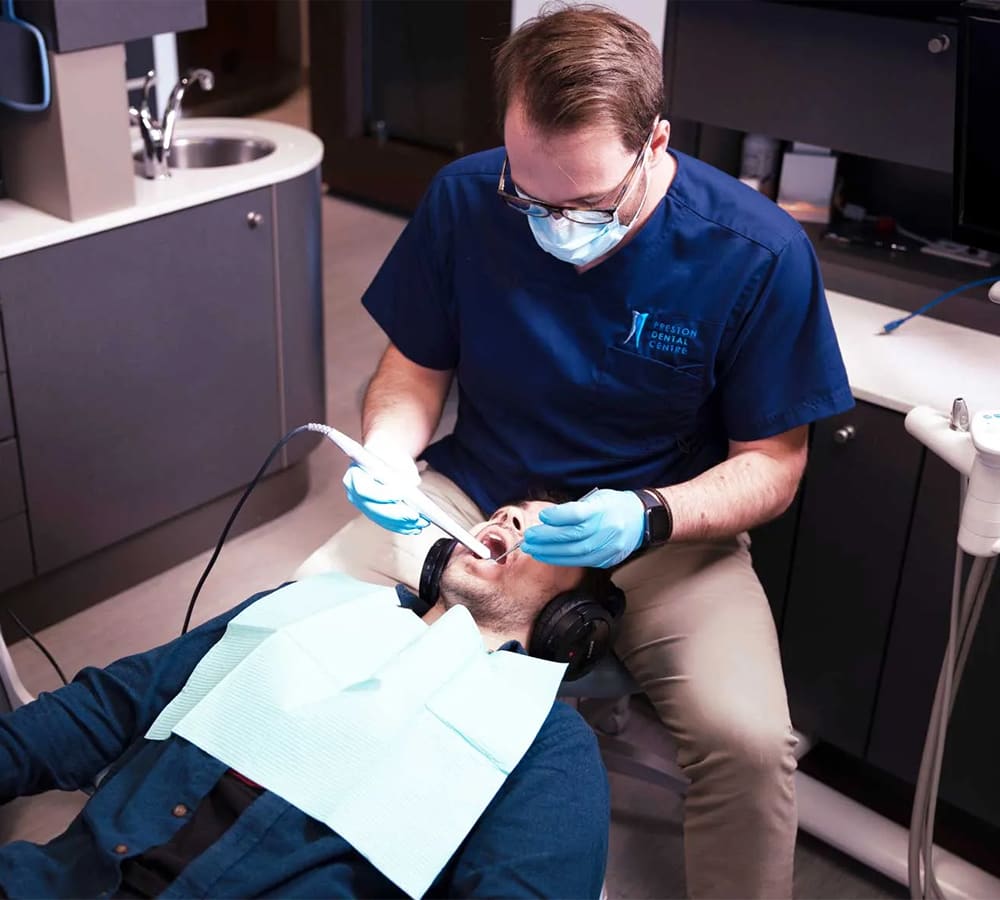
Oral Examinations
You should be attending oral exams twice a year. This way, your dentist can identify oral heath concerns early, while they are most treatable.
During your exam, your dentist will likely take dental X-rays so that they can see what is going on below the gum line. They will also take a close look at your teeth, gums, jaw and bite, and see if there are any issues that need addressing.
Oral Cancer Screening
Oral cancer can affect any part of the mouth and surrounding tissues, so your dentist will check your neck, face, lips, tongue, throat, and gums.
At Preston Dental Centre, we use a VELscope® oral cancer screening device to identify any abnormalities that could be hard to detect with the naked eye.
Oral Health Care at Home
To keep your smile healthy between dental appointments, be sure to brush your teeth twice a day for two minutes each time, and floss at least once a day.
Dental Hygiene Cleaning
During your dental appointment, a hygienist will perform a thorough cleaning of your teeth and gums to treat and prevent disease.
They will start by using a scaler to remove plaque and tartar buildup, then they will use a polisher and a coarse toothpaste to remove any stains. The cleaning will end with your hygienist flossing your teeth and gums.
Fluoride Treatment
If you are at a high risk of tooth decay, your dentist may also recommend a fluoride treatment. Fluoride is a natural mineral that can help rebuild your tooth enamel to prevent or reverse tooth decay.
Fluoride can also be used as an effective treatment for dry mouth, as it can lower the acidity of your mouth and fight bacterial growth.